End-to-End Revenue Cycle Management Services

Optimized Revenue Cycle Management
In today’s healthcare landscape, efficient Revenue Cycle Management (RCM) is essential to maintain financial stability and deliver high-quality patient care. Studies reveal that up to 25% of potential medical revenue is lost due to denied claims, billing delays, and administrative errors — challenges that can seriously impact your practice’s growth.
Our comprehensive RCM services are designed to eliminate these gaps. From real-time eligibility verification and accurate medical coding to fast claim submissions and proactive follow-ups, we ensure your billing process runs smoothly and efficiently. This approach minimizes claim rejections, recovers lost revenue, and boosts your cash flow — all while maintaining full compliance with healthcare regulations.
By improving collection rates, reducing administrative burdens, and lowering operational costs, we help your practice focus on what truly matters: delivering exceptional patient care. Whether you’re an independent physician or a growing healthcare organization, our smart revenue cycle strategies provide the stability, scalability, and profitability you need to succeed in today’s competitive market.

4 Best Practices for Boosting Medical Practice Revenue
Increasing revenue in a medical practice requires more than excellent patient care — it demands strategic planning, accurate documentation, and streamlined workflows. At SA Care Consultancy, we help healthcare providers refine their processes to improve cash flow, reduce denied claims, and strengthen financial stability.
By focusing on front desk efficiency, accurate coding, effective denials management, and minimizing unnecessary write-offs, your practice can achieve sustainable growth while staying focused on delivering quality patient care.

Enhance Front Desk Training
Train staff to collect accurate insurance and demographic details, verify coverage before appointments, and collect co-pays at the time of service to reduce claim denials and improve cash flow.
Improve Documentation and Coding
Use specific ICD-10-CM codes that match clinical documentation, educate providers on detailed record-keeping, and avoid vague terms to prevent claim rejections and delays.
Refine Denials Management
Establish clear protocols for tracking claims, update staff on payer policy changes, and improve communication to ensure timely and accurate payments.
Reduce Unnecessary Write-Offs
Investigate claim denials before writing them off, implement an appeals process, and submit strong documentation to recover more payments.
Systematic RCM Process
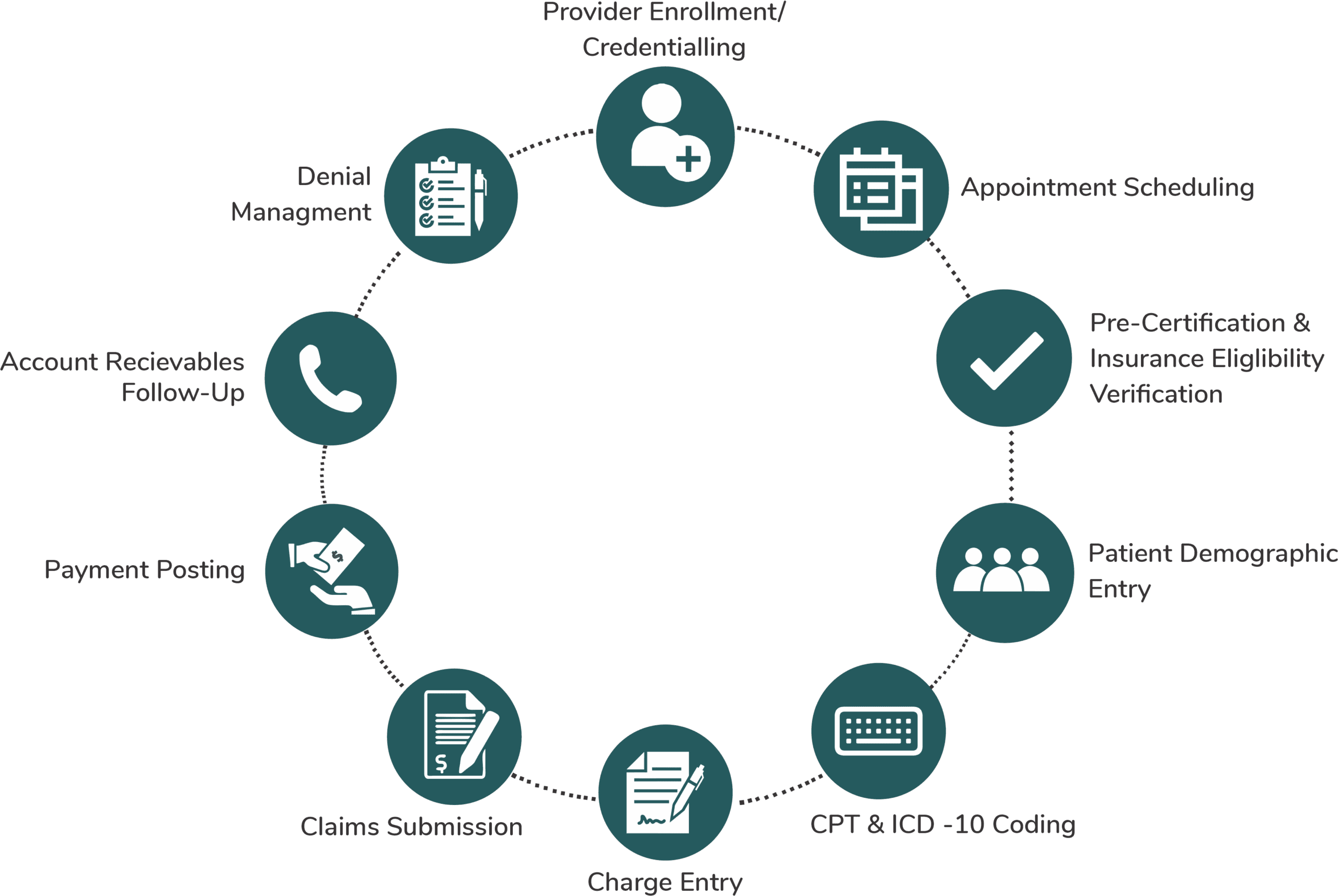
Daily RCM Insights
At iSolve RCM, we provide cost-effective and comprehensive Revenue Cycle Management services that give you a clear view of your practice’s financial health every day. Our end-of-day reports help you track key figures, identify trends, and make informed decisions to improve cash flow and maximize revenue.Our RCM services ensure that your claims & denials are thoroughly worked on and always result in maximum reimbursement. We employ ingenious machine-learning algorithms that help predict revenue streams and risk factors. Our process is also equipped with artificial intelligence that aids in automation and scalability and customization. From Pre-Certifications to Final payment posting & reporting, we take care of it all.

boost your revenue with Best RCM services
Specialities We Do Credentialing For
Healthcare professionals can take advantage of our experience in a wide range of specialties by working
with SA Care Consultancy. We ensure that your billing and coding requirements are met accurately and promptly.
Scribe Align specializes in a range of medical billing and coding specialties, including:
Cardiology
Neurology
Oncology
Orthopedic
Dermatology
Urology
Family Medicine
Internal Medicine
Psychiatry
Radiology
Nephrology
Anesthesia
Why Choose Us for RCM Services

Rapid Revenue Recovery
25 Days

First-Pass Resolution
99 %

Denial & Rejection
5 % - 10%

Short Turnaround Time
24 Hours

Electronic Claim
95%

Electronic Payment
95%

Client Retention
100 %

Revenue Increase
30%
Trusted Softwares You’ll Recognize
























What Our Clients Says
Our clients trust us to deliver results — here’s what they have to say about their experience.
Their RCM support made patient payments smooth and predictable—we finally have consistent cash flow.
My clinic’s website started ranking locally in just two months, and appointments are flowing in.
They helped me turn my idea into a real launch with clear steps and supportive guidance.
Outsourcing admin tasks freed up our time, and new partnership leads started coming in.
Our website is fast, clean, and easy for patients to use—exactly what we needed.
Accurate coding eliminated billing errors and helped us avoid denials.
They got our providers credentialed quickly—claims started processing sooner than expected.
Their process system made our billing cycle clear and easy to manage.
– Jessica Turner
Eligibility checks now happen upfront—no surprises, no delays.
They helped chase payments effectively—AR days dropped noticeably.
– Priya Singh
Denied claims got resolved fast—revenue bounced back immediately.
– Emily Jackson
The help desk is responsive and scheduling errors are now rare.
– Michael Lee
Their authorization follow-ups saved us so many denied pre-authorizations.
Their reports are tailored to our needs—easy to understand and very useful.
Stronger RCM, Stronger Practice
Don’t let revenue leakages hold you back. Our RCM solutions streamline billing, claims, and collections so your practice runs smoothly and grows consistently.
frequently asked question
Revenue Cycle Management is the process of managing a healthcare provider’s billing, coding, claims, and payment collection to ensure smooth cash flow and reduced revenue loss.
Efficient RCM helps minimize denied claims, speed up reimbursements, improve financial health, and allow you to focus on patient care instead of administrative work.
We provide end-to-end RCM services including eligibility checks, accurate coding, claim submissions, denials management, and reporting to optimize your revenue collection.
Yes, our team investigates denied claims, files appeals when necessary, and ensures proper documentation to recover maximum possible payments.
Far far away, behind the word mountains, far from the countries Vokalia and Consonantia, there live the blind texts.
Yes, we provide daily and monthly reports so you always know where your practice’s finances stand and can make informed decisions.
